It sounds like a distant threat—bacteria so resistant to antibiotics that they become nearly impossible to treat. But scientists at the University of the Philippines (UP) Manila say antimicrobial resistance, or AMR, is not a problem for the future. It is already here, already in the food Filipinos eat and the drinks they buy on the street.
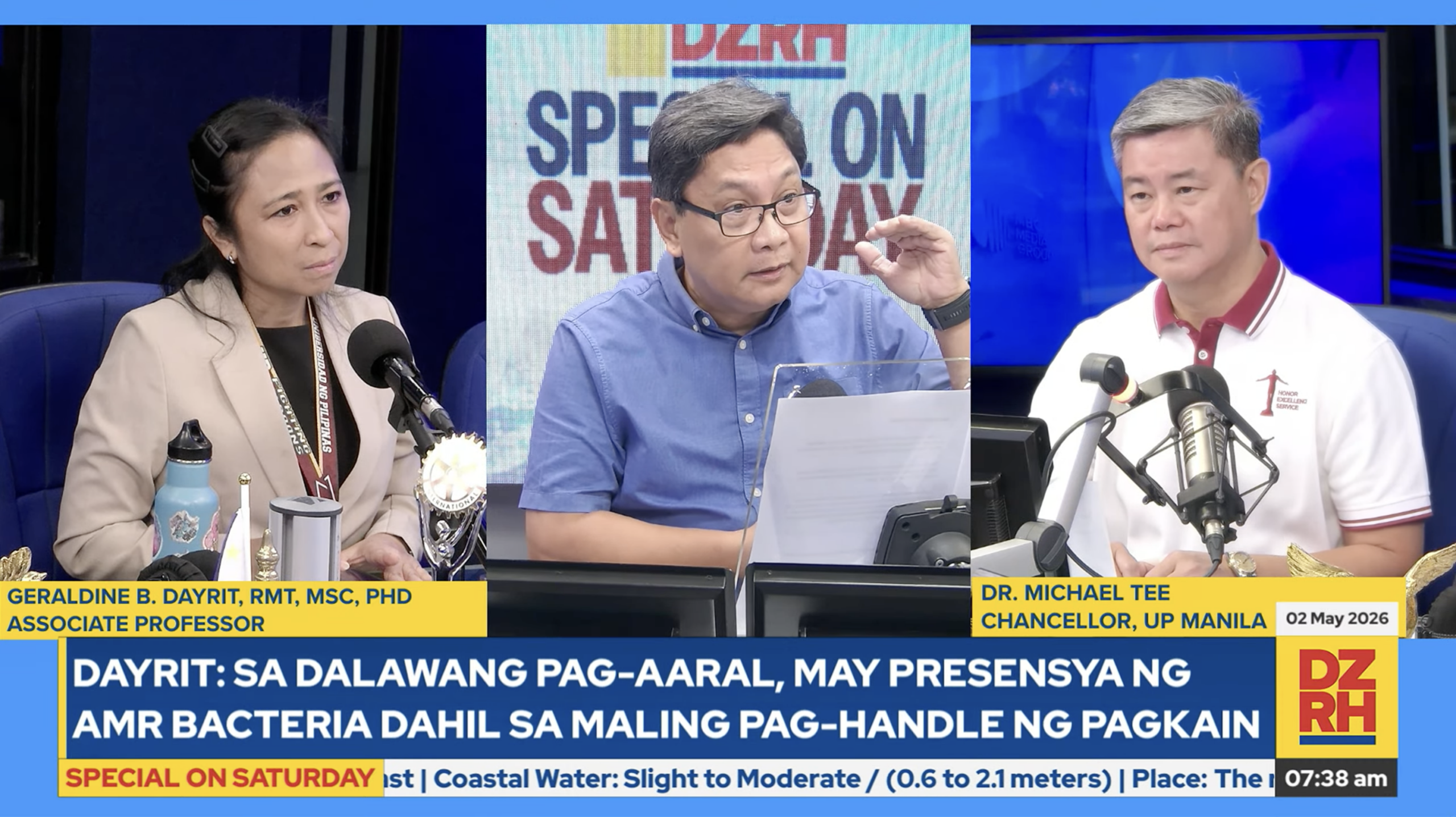
A UP Manila study conducted in 2024 to 2025 found drug-resistant bacteria in all 12 sampled palamig stalls in Tondo, Manila—detected in the beverages, the ice, the cups, and the palms of the vendors who served them. The findings, presented publicly on DZRH News program “Special on Saturday” on May 2, put a local face on a global health crisis that experts warn could reshape medicine as we know it by mid-century.
“Sa 2050, maaaring ang antimicrobial resistance na ang magiging dahilan kaya lalong lalala ang mga sakit ng ating mga kababayan, na maaaring magkaroon na tayo ng hirap gamutin ang mga common infection,” UP Manila Chancellor Dr. Michael Tee said.
The warning is not new to the global health community. A projection cited in the UP Manila research presentation states that AMR-causing superbugs could eventually kill more people than cancer—a sobering benchmark given that cancer claims nearly 10 million lives per year worldwide, or nearly one in six deaths, according to WHO data. The threat is driven by the rapid pace at which bacteria develop resistance compared to the slow, expensive process of developing new antibiotics.
“Mabagal mag-develop ng gamot, pero mag-develop ng antimicrobial resistant strain ng mga bacteria ay napakabilis,” Tee said, noting that while new drugs can take 5 to 15 years to reach the market, bacteria can develop resistance in as little as six months.
AMR occurs when bacteria evolve to survive antibiotic treatment—rendering medicines that once worked less effective or entirely useless. This happens through multiple pathways: patients who take antibiotics unnecessarily, patients who do not complete their full course of medication, and the widespread use of antibiotics in food production—in poultry, pigs, and aquaculture—which introduces resistant bacteria into the broader environment through animal waste and water systems.
“Uminom ka ng gamot nang mali, o kaya sa paligid mo… ‘yung mga pagbigay ng antibiotics, binibigay ‘yan sa mga manok,” Tee explained. “‘Yung feeds na napupunta sa tubig, napupunta sa ating mga river. In the process, pumapasok sa katawan mo.”
This is the core of what scientists call the One Health framework—the recognition that human health, animal health, and environmental health are inseparable. AMR does not originate only in hospitals or pharmacies. It circulates through the food supply, waterways, and the everyday environments where people live and eat.
UP Manila Associate Professor Dr. Geraldine Dayrit, who led the study into palamig stalls, said the presence of AMR bacteria in street food is particularly alarming because of the resistance genes they carry—genes that can transfer between bacteria and spread to other people. “Bukod po sa bacteria, may resistance genes po, ang tawag po dito ay ‘yung pwede pong mai-transfer nang madalian sa ibang tao,” she said.
The practical consequence is this: a Filipino who consumes AMR-carrying bacteria and later falls ill may find that the antibiotic their doctor prescribes does not work as expected. “Itong bacteria na kahit pinainom ka ng ordinaryong antibiotic, maaring walang bisa o kulang sa bisa,” Dayrit said.
The study found AMR bacteria not only in palamig drinks and ice, but also in ready-to-eat street food including kwek-kwek, sawsawan, raw seafood such as kinilaw, fresh produce sold as salads, and improperly processed poultry. Dayrit also noted that fruits eaten without washing — including those that appear clean or are store-wrapped — can carry resistant bacteria as well. “Kinakain natin diretso po ‘yan,” she said.
Tee contextualized the public health stakes with data from the UP Manila College of Public Health’s (CPH) Medical Atlas, noting that lower respiratory tract infections—one category of illness where AMR poses a direct treatment risk—rank second among causes of death in the Philippines in terms of years of life lost. Diarrhea, a common outcome of consuming contaminated food and water, ranks 19th among the top causes of age-standardized death in the country.
“Una, ito ay isang preventable o maiiwasan na problema,” Tee stressed. He called for barangay-level vendor training, environmental sanitation enforcement at selling areas, and broader public awareness—arguing that the cost of prevention is far lower than the cost of treating communities where AMR has taken hold.
The KAP—Knowledge, Attitudes, and Practices — component of the UP Manila research, which surveyed food handlers and vendors across Metro Manila market stalls, has already been published in a peer-reviewed journal. Dayrit said the data is available for use by government agencies and LGUs as a policy basis—a starting point, she said, for action that does not require waiting for further study.